Article by Stacey J. Butler
Graphic design by Ingrid Barany
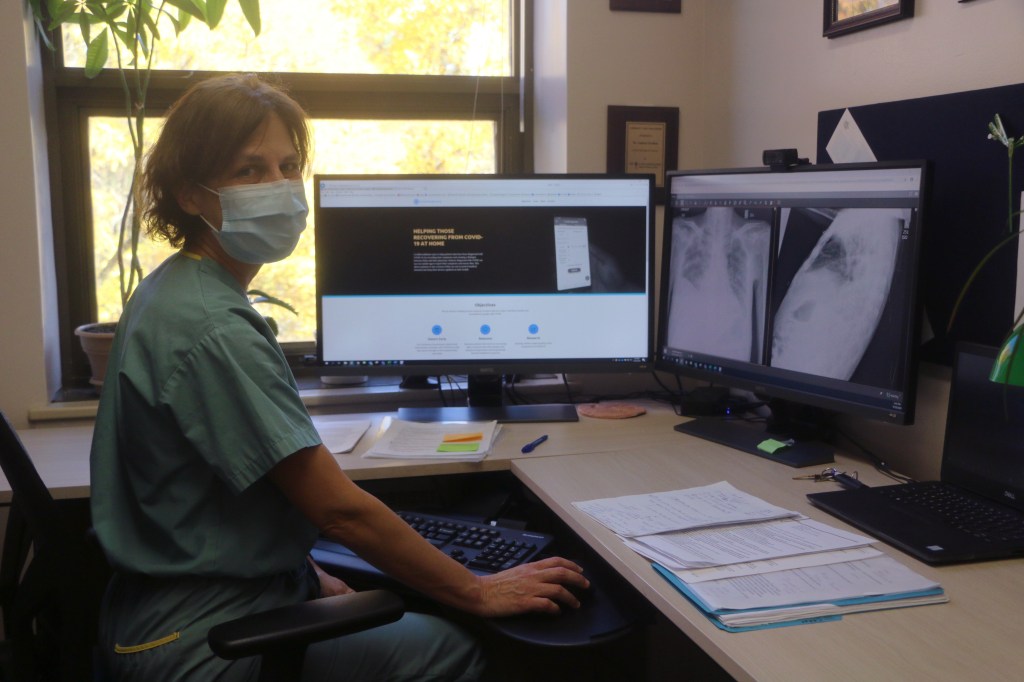
Like many of Toronto’s renowned respiratory disease researchers, Dr. Andrea Gershon feels it is her duty to study the emerging coronavirus. As lead of the CanBREATHE–Lung Health research group, her knowledge in the field of Respirology is highly relevant to COVID-19. An active member of both the Canadian Thoracic Society and the Canadian Respiratory Research Network, Dr. Gershon has years of experience conducting clinical and population health research with the common goal of improving health outcomes for people living with chronic respiratory disease. She is also a staff Respirologist at Sunnybrook Health Sciences Centre and has been working on the front-lines during the COVID-19 pandemic. Dr. Gershon has seen first-hand how healthcare workers have stepped up and supported each other despite the fear and anxiety that comes with their heightened risk of exposure to the novel coronavirus.

Associate Professor, Department of Medicine, University of Toronto
Research Director & Staff Respirologist, Division of Respirology, Sunnybrook Health Sciences Centre
Scientist, Evaluative Clinical Sciences, Trauma, Emergency & Critical Care Research Program, Sunnybrook Research Institute
Senior Core Scientist & Lung Health Lead, ICES
Photo Credit: Dorsa Derakhshan
Throughout the pandemic, we have often heard the expression “these are unprecedented times”, but the early days of the COVID-19 pandemic felt like déjà vu for Dr. Gershon. In 2003, she was a young mother and a medical resident, ‘moonlighting’ at Scarborough Grace Hospital. She was asked to assess a patient in the emergency room who presented with an abnormal chest x-ray. No masks, no gowns–they were completely unaware that they were treating the first patient with severe-acute respiratory syndrome (SARS) in Canada. All they knew was that the patient’s relatives had also fallen ill, and one was in the intensive care unit (ICU) where Dr. Gershon later attended to a code blue–a medical emergency. As the investigation continued, they recognized the severity of the illness, and quickly became aware of the possibility that they were facing a new infectious disease. Dr. Gershon’s story highlights how the early days of the COVID-19 pandemic resembled the SARS era. The initial response was similar – quarantine anyone who may have been exposed. Dr. Gershon recalls being put in quarantine nearly a week after she treated the first SARS patient. To simply label this experience as frightening would be an understatement, yet it is one that many Canadians are all too familiar with today.
Dr. Gershon felt helpless in the early days of the COVID-19 pandemic. She wanted to find a way to apply her relevant experience in respiratory disease and accelerate COVID-19 research. While looking for ways to pivot their research to study the new coronavirus, Dr. Gershon and her team realized they had already developed the perfect tool to monitor COVID-19 patients. Ironically, they had been testing this tool in patients with chronic respiratory disease at the beginning of the pandemic, but their study was put on hold when all clinical research came to a grinding halt. Along with an interdisciplinary team of clinicians and computer scientists, namely Dr. Robert Wu, Dr. Eyal de Lara, and Dr. Daniyal Liaqat, they had already created a smartphone application that allows health care providers to remotely monitor a patient’s health. With the support of the Canadian Institute of Health Research (CIHR), and the Physicians’ Services Incorporated (PSI) Foundation, they are now using this technology to quickly gather data that can improve our understanding of COVID-19 symptoms and disease progression.
One of the current issues with COVID-19 is not knowing when patients, who are isolating at home, need to be transitioned to hospital-based care. When someone tests positive with COVID-19 they are simply instructed to self-isolate and seek medical attention when needed. Not only can this leave patients in a state of panic, worrying about when their health will deteriorate, it also has the potential to overwhelm the healthcare system with unnecessary emergency department visits and hospitalizations. Dr. Gershon and her team’s COVIDFree@Home project uses cutting-edge technology to monitor the health of COVID-19 patients who are isolating at home. The team hopes to employ artificial intelligence and machine learning models to predict when patients need to be hospitalized. This technology allows them to do all of this without going within six feet of a patient.
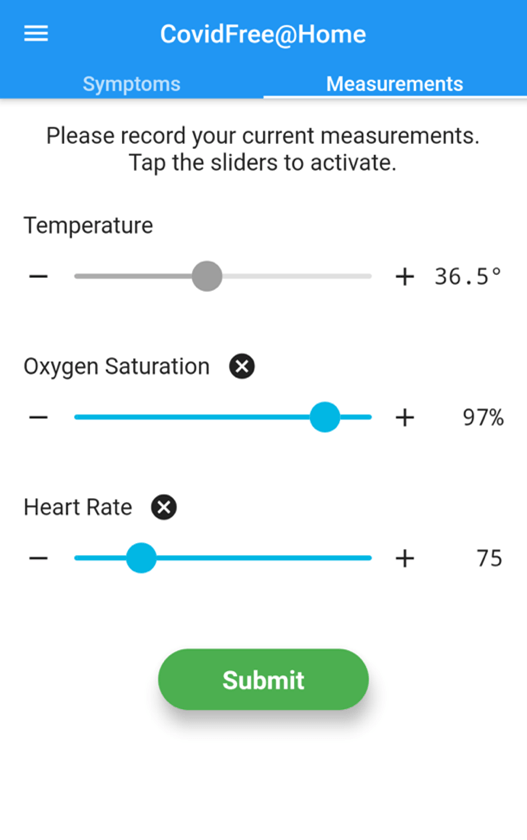
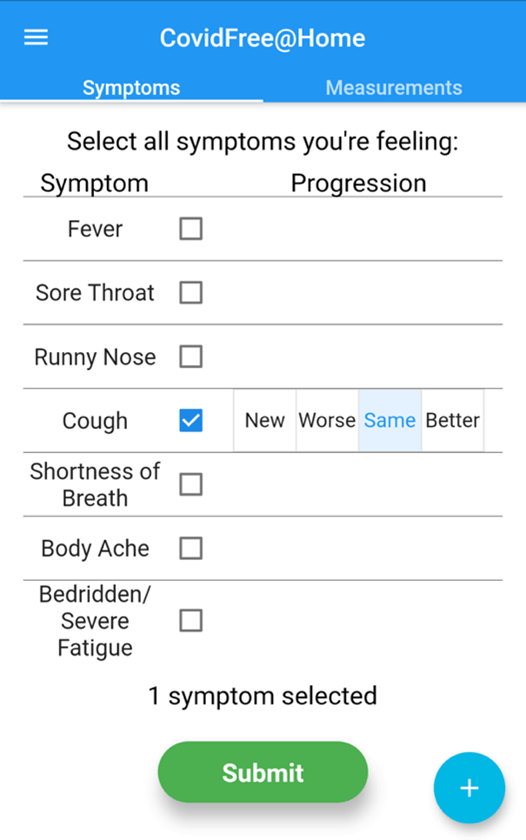
The COVIDfree@Home study is enrolling patients who test positive for COVID-19 and are self-isolating in the community. Study participants are recruited from emergency departments and clinics which receive referrals from COVID-19 screening centres at the University Health Network and Sunnybrook Health Sciences Centre. The team hopes to extend the research study to enroll patients from centres in other COVID-19 hot-spots, such as the Humber area and Peel region. The study participants are mailed an oximeter and thermometer to measure their blood oxygen levels and temperature at home. They are asked to use an app on their smartphone to record their symptom severity, oxygen saturation, and temperature twice daily. The app can even measure respiratory rate and detect coughs, using advanced algorithms developed by the research team. Patients are monitored during the peak of their infection for two weeks.
The research team will use this data to predict the point at which patients need to be hospitalized. The benefit is obvious–it allows a large group of patients to be monitored remotely, in real-time, by only a small number of healthcare professionals. Widespread use of this tool will ultimately put less strain on the healthcare system, which has been the goal since the start of the pandemic. At this point, the only tools we have to mitigate the spread of COVID-19 and prevent our healthcare systems from being overwhelmed are abiding by social distancing protocols and other public health guidelines.
Currently, our brave healthcare workers have limited tools to treat patients with COVID-19. Preliminary research worldwide has assisted in identifying vulnerable groups with worse outcomes and improving hospital-based care, but little is being done for patients in the community. Research projects like Dr. Gershon’s COVIDFree@Home are vital to improve our understanding of COVID-19, ensure patients are safe when isolating at home, and help the healthcare system adapt and move forward.

You must be logged in to post a comment.